Frank Vinluan
MedCityNews.com
Originally posted 1 April 24
A software app that modifies behavior through a series of lessons and exercises has received FDA clearance for treating patients with major depressive disorder, making it the first prescription digital therapeutic for this indication.
The product, known as CT-152 during its development by partners Otsuka Pharmaceutical and Click Therapeutics, will be commercialized under the brand name Rejoyn.
Rejoyn is an alternative way to offer cognitive behavioral therapy, a type of talk therapy in which a patient works with a clinician in a series of in-person sessions. In Rejoyn, the cognitive behavioral therapy lessons, exercises, and reminders are digitized. The treatment is intended for use three times weekly for six weeks, though lessons may be revisited for an additional four weeks. The app was initially developed by Click Therapeutics, a startup that develops apps that use exercises and tasks to retrain and rewire the brain. In 2019, Otsuka and Click announced a collaboration in which the Japanese pharma company would fully fund development of the depression app.
Here is a quick summary:
Rejoyn is the first prescription digital therapeutic (PDT) authorized by the FDA for the adjunctive treatment of major depressive disorder (MDD) symptoms in adults.
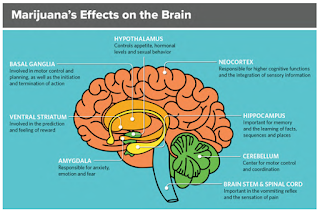
Rejoyn is a 6-week remote treatment program that combines clinically-validated cognitive emotional training exercises and brief therapeutic lessons to help enhance cognitive control of emotions. The app aims to improve connections in the brain regions affected by depression, allowing the areas responsible for processing and regulating emotions to work better together and reduce MDD symptoms.
The FDA clearance for Rejoyn was based on data from a 13-week pivotal clinical trial that compared the app to a sham control app in 386 participants aged 22-64 with MDD who were taking antidepressants. The study found that Rejoyn users showed a statistically significant improvement in depression symptom severity compared to the control group, as measured by clinician-reported and patient-reported scales. No adverse effects were observed during the trial.
Rejoyn is expected to be available for download on iOS and Android devices in the second half of 2024. It represents a novel, clinically-validated digital therapeutic option that can be used as an adjunct to traditional MDD treatments under the guidance of healthcare providers.